TVP: A Cheaper and Effective Alternative to TURP
Departments of Minimally Invasive Therapy,
London Clinic, Devonshire Place, London W1N & United Medical and Dental
schools of
Guy's & St. Thomas's Hospitals, London SE1 7RT.
MS Nathan
MS, FRCS, DUrol.
Associate Lecturer, Department of Minimally Invasive Therapy,
United Medical & Dental Schools of Guy's & St.Thomas's, New Guy's
House,
London SE1 7RT
JEA Wickham
MS, MD, BSc, FRCS, FRCP, FRCR
Senior Research Fellow & Honorary Consultant
Department of Minimally Invasive Therapy
United Medical & Dental Schools of Guy's & St. Thomas's,
New Guy's House, London. SE1 7RT.
MS Nathan
Department of Minimally Invasive Therapy
United Medical & Dental Schools of Guy's & St. Thomas's,
New Guy's House, London. SE1 7RT.
TVP: A Cheaper and Effective Alternative to TURP
Summary
Transurethral electrovaporisation of the prostate (TVP) is a new minimally invasive procedure to treat enlargement of the prostate. It was the aim of this study to compare the efficacy, postoperative morbidity and costs of transurethral resection (TURP) with TVP of the prostate. Forty men requiring a transurethral resection of the prostate over a period of 12 months were randomly selected to undergo either TURP (20 men) or TVP (20 men). The improvement in the urinary symptoms and peak urinary flow of the two groups were measured before and after surgery. The postoperative morbidity, hospital stay, operating time and the costs of the two procedures were analysed in detail.
Both TURP and TVP were found to have the same efficacy in relieving prostatic symptoms and obstruction with a successful surgical outcome in 85% of the men. The mean hospital stay for the TVP group (1.85 days) was significantly lower than the TURP group (3.5 days) as were the postoperative bladder irrigation and catheterisation time (p= <0.0001). TVP was significantly cheaper than TURP due mainly to the reduced hospital stay, blood transfusions and cost of bladder irrigants. The overall morbidity was less for the TVP group (10%) in comparison to TURP (15%).
TVP is as effective as TURP in relieving prostatic symptoms while being less morbid and cheaper with a shorter hospital stay: probably a better alternative to TURP.
Keywords
Transurethral resection of the prostate; Transurethral electrovaporisation of the prostate; success; morbidity; costs.
IntroductionTransurethral resection of the prostate (TURP) is the gold standard for treatment of the enlarged prostate but the associated morbidity has led to the investigation of various therapeutic alternatives. Transurethral electrovaporisation of the prostate (TVP) is a new technique that is undergoing trials in various centres and preliminary reports have indicated a success rate comparable to TURP (1). TVP uses a grooved cylinder instead of the conventional loop used in TURP with higher diathermy power settings. Extensive work done by Bush et al have shown that such a mechanism effectively vaporises the tissue it comes in contact and dessicates the deeper tissues (2). To assess whether TVP would be a better alternative to TURP we decided to randomly compare the two procedures with the following objectives:
- To assess their objective and symptomatic success rates.
- To study and compare resection or vaporisation time, haemostasis
time and theatre costs.
- To compare the incidence of various postoperative complications and
the overall morbidity rate.
- To compare the duration of hospital stay and evaluate the total cost of the 2 procedures.
Forty men requiring TURP were randomly selected to undergo either TURP or TVP. Their symptoms (IPSS-S) and quality of life (IPSS-L) assessment were graded by the The International Prostate Symptom Score technique. Patients who had undergone previous prostate operations or those with known neuropathic bladders were excluded from the trial. Similarly patients with indwelling catheters and on anticoagulant therapy were also excluded while those on antiplatelet therapy were asked to stop taking their medication a week prior to their procedure if they were having a TURP.
Preoperative investigations in all the men included uroflowmetry, abdominal ultrasound and transrectal ultrasound (TRUS) of their prostates. All the operations were done by JEAW using a 24Ch continous resectoscope and its loop for a TURP or a 25Ch ACMI Circon resectoscope and the VaporTrodeTM for TVP. In all the cases a Valleylab Force-2 diathermy machine was used with the current set to 120watts cutting and 60watts coagulation for TURP and 200watts cutting and 40watts coagulation for TVP. Two hundred milligrams of intravenous Nettilin was given and resection or vaporisation done to the crossing white fibres of the surgical capsule. Haemostasis was adequately achieved and a 3-way size 20F Porges catheter was placed at the end of the procedure. The duration of the resection or vaporisation time and the haemostasis time in the operating theatre was noted. The length of postoperative bladder irrigation and catheterisation time and the entire hospital stay were recorded. The number of irrigant bags used per and postoperatively, bladder washouts and blood transfusions were carefully noted.
All the patients were followed up 4,8 and 12 weeks after their surgery and symptoms scored. Postoperative uroflowmetry was done on all the patients and their urine residual volumes measured. All statistical analysis were done using the student's paired two tailed 't' test.
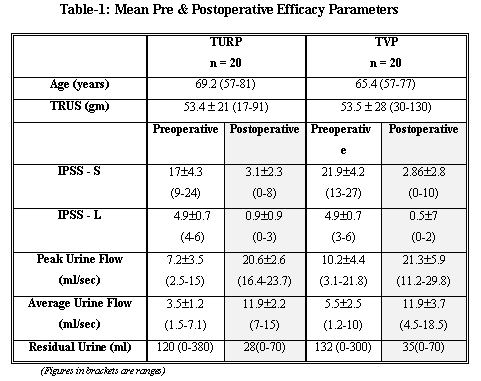
ResultsThe preoperative criteria of the 40 men enrolled for this study is shown in Table - 1. It can be seen that the two groups matched evenly for their age, prostate size, symptoms and the objective evidence of obstruction.
Clinical EfficacyThe postoperative improvement in the patients' symptoms and quality of life can be seen in Figure-1. Although there was significant postoperative improvement in the IPSS-S and IPSS-L (p=<0.0001) scores in both TURP and TVP groups there was little difference between the two groups. Patients with a postoperative IPSS-S of more than 5; a IPSS-L of more than 3 or a peak flow rate of less than 15ml/sec were considered as surgical failure. Three men in the TURP group and two in the TVP group had IPSS-S and IPSS-L scores more than 5 and 3 respectively. The mean postoperative urinary peak flow rate and the Average flow rates were 20.6 ml/sec and 11.9 ml/sec respectively in the TURP group while similar results of 21.3 ml/sec and 11.9 ml/sec were noted in the TVP group. The mean postoperative urinary residual volumes were 27.6ml and 35ml in the TURP and TVP groups respectively. Table-1. Two patients in the TURP group and three patients in the TVP group had peak flow rates less than 15ml/sec.
Postoperative MorbidityTable-2 shows the incidence of the various postoperative complications noted in the two groups and their duration. Two men in the TURP group had postoperative blood loss requiring transfusions while none of the patients in the TVP group required blood transfusions. At the first month follow up 60% of the patients in the TURP group and 20% in the TVP group complained of diurnal urinary frequency which dramatically reduced in the TURP group during subsequent visits. Dysuria after 8 weeks of surgery was noted in 5% of the patients in both groups but persistent dysuria after 3 months was noted in one patient following TURP. Postoperative urinary tract infection was found in 3 patients from the TURP group while 2 men in the TVP group developed this problem. One patient in the TURP group developed postoperative clot retention which settled on conservative management. Transurethral resection syndrome was not observed in any patient and none required re-operation.
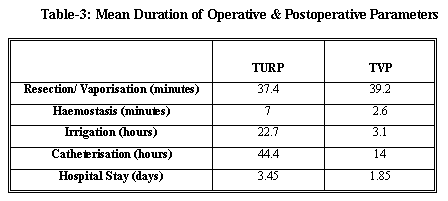
DurationTable-3 shows the duration of the various per and postoperative parameters noted in this study. The mean hospital stay (less than 2 days) for the TVP group was significantly lower (p= <0.0001) than the TURP group (3 and a half days). Similarly the catheterisation and the irrigation time were significantly lower for the TVP group with little difference in the resection or vaporisation time. The mean operative time was 44.4 minutes for the TURP group in comparison to 41.8 minutes for the TVP group due mainly to the longer haemostasis time.
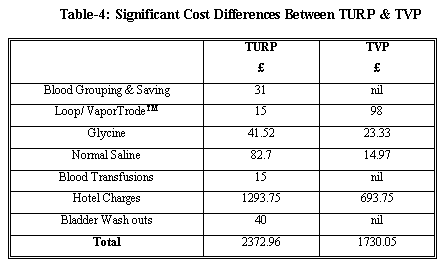
CostsThe costs of the two procedures were recorded in detail and the significant differences are shown in Table-4. In total TURP cost 44% more than TVP mainly due to the hotel bills engendered by the increased hospital stay, cost of irrigant and preoperative grouping and saving of blood. The mean cost of normal saline and glycine irrigant fluids were 81% and 43% respectively less in the TVP group, savings which were negated by the cost of the VaporTrodeTM.
DiscussionElectrovaporisation of the prostate has become feasible with a better understanding of the passage of electric current into the tissues and development of the VaporTrodeTM. The search for an alternative to TURP has continued mainly to reduce the postoperative morbidity, hospital stay and cost of the procedure. Any alternative management to TURP should have the same or even better success rate than TURP. It would be advantageous if the procedure is non-invasive or atleast not more invasive than TURP but also allowing prostate glands larger than 60gms to be treated. An ideal alternative should be easy to learn, quicker to perform, cost effective and reduce hospital stay. Most importantly it should be associated with less morbidity and mortality than TURP.
The symptomatic (85%) and objective (90%) success rates of the patients in the TURP group of this study are similar to other reports (3,4). Similar results are noted in the TVP group where 90% of the men reported significant postoperative improvements in their symptoms and quality of life and 85% of the men showed marked improvements in their peak and average urinary flow rates similar to other reports (5). There was no appreciable difference in the symptomatic (p= 0.873) or objective (p= 0.657) success rates among the two groups indicating that TVP is as effective as TURP in relieving prostatic symptoms and obstruction.
The mean operating time for TVP was 41.8 minutes similar to that of Kaplan and Te (40.3 minutes) who treated patients with a mean prostate size similar to this study (6). In comparison to TURP the mean operating time for TVP was shorter mainly due to the saving on the haemostasis time, the mean resection and vaporisation time being nearly the same for both the groups (p= 0.681). On average the TURP patients required bladder evacuation at surgery 4 times to clear out clots and chips while the TVP patients required this only once. The mean hospital stay was significantly shorter (p= <0.0001) for the TVP group, saving nearly £625 per patient in comparison to TURP. Although the mean hospital stay for the TVP group was 1.85 days 5 patients were admitted and discharged in less than 36 hours and 2 within 24 hours almost as day case surgery.
The main clinical differences were in the postoperative period for the 2 groups where the mean saline irrigation time and postoperative catheterisation time for the TURP group were 22.7 and 44.3 hours respectively in comparision to the TVP group where it was significantly less (p= <0.0001). The mean postoperative saline irrigation time (3 hours) and catheterisation time (14 hours) in the TVP group was similar to other studies (6). This reduction was mainly due to the reduced postoperative bleeding that occurred after TVP in comparison to TURP leading to a considerably reduced postoperative stay in hospital with a very significant saving in the overall cost of the operation. Four men in the TURP group required a total of 10 bladder wash outs in contrast to the TVP group where this was not needed in any patient.
The morbidity rate for the TURP group was 15% similar to other reports (7,8). The chief cause of this was postoperative bleeding requiring blood transfusions, bacteraemia and urinary tract infection. The morbidity rate for the TVP group was 10% due mainly to urinary tract infection and persistent postoperative dysuria. At the four weeks follow up nearly two-thirds of the patients in the TURP group complained of diurnal frequency in comparision to 20% of the men in the TVP group. This was felt to be secondary to the increased fluid intake advised to flush the bladder. As postoperative bleeding is minimal in the TVP group majority of the patients returned to their normal drinking habits within a week after surgery.
Excluding professional charges the mean cost of TURP was £2373 per patient of which the hotel charges accounted for nearly 50% of the cost of TURP similar to other studies (9) and made the procedure significantly costlier in comparision to TVP (£1730). The cost of irrigant fluid and the grouping and administration of blood were significantly (p= <0.0001) more costlier in the TURP group while the cost of the VaporTrodeTM was much costlier than the ordinary loop. None of the patients in the TVP group required their antiplatelet regime altered thus reducing the risk of potential cardiac or cerebral ischaemia. The risk of absorption of irrigant fluid is minimal in TVP and large prostate glands can be safely operated (10). In this study the size of the prostate gland in 3 men was larger than 70grams and all of them had a successful outcome.
ConclusionThe objectives set out in this study were to compare and assess TVP with TURP particularly regarding the efficacy, morbidity rate, duration of hospital stay and cost. In line with the above four main criteria for an alternative therapy to TURP this study shows that TVP could be a better alternative as it has a lower postoperative morbidity rate, reduced hospital stay, is cheaper and has the same short term efficacy of TURP. The benefits of TVP over TURP are summarized in Figure-2. If multicentric long-term comparative studies show the same success rate of TURP then TVP can be considered as the ideal alternative to the time tested conventional TURP.
References
- Kaplan SA, Te AE. Transurethral electrovaporisation of the prostate:
A novel method for treating men with benign prostatic hyperplasia. Urol
1995; 45: 566-572.
- Bush IM, Malters E, Bush J. Transurethral vaporisation of the prostate
(TVP): New horizons. J Soc Min Invas Ther 1993; 2: 93.
- Kuo H, Chang S, Hsu T. Predictive factors for successful surgical
outcome of BPH. Eur Urol 1993; 24:12-19,.
- Montorsi F, Guazzoni G, Bergamaschi F, Consonni P, Matozzo V, Barbieri
L, Rigatti P. Long term clinical reliability of transurethral and open
prostatectomy for benign prostatic obstruction: A term of comparison
for nonsurgical procedures. Eur Urol 1993; 23: 262-266.
- Te AE, Reis R, Kaplan SA. TVP: A new modification of TURP. Contemp
Urology May 1995; 74-83.
- Kaplan SA, Te AE. A comparative study of transurethral resection of
the prostate using a modified electro-vaporising loop and transurethral
laser vaporisation of the prostate. J Urol 1995; 154: .
- Mebust WK, et al. Transurethral prostatectomy: Immediate and post-operative
complications. A cooperative study of 13 participating institutions
evaluating 3885 patients. J Urol 1989; 141:243-247.
- Melchior J, Valk WL, Foret JD, Mebust WK. Transurethral prostatectomy:
Computerized analysis of 2223 consecutive cases. J Urol 1974; 112:634-646,.
- Drummond MF, McGuire AJ, Black NA, Petticrew M, McPherson CK,. Economic
burden of treated BPH in the U.K. Br J Urol 1993; 71:290-296.
- Te AE, Kaplan SA. Transurethral electrovaporisation of the prostate TVP: An electrosurgical advancement of the standard TURP. Curr Surg techniques Urol 1995; 8:1-8.